SPECIAL EDITION: Leading expert and STOP Member Allison Sylvetsky, PhD, discusses the science of non-nutritive sweeteners and their role in obesity management.
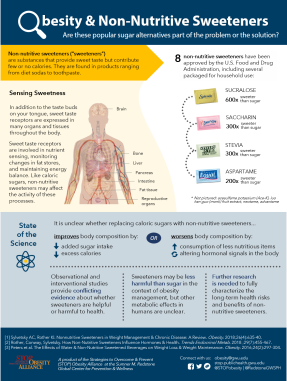
If you brushed your teeth with toothpaste, chewed a multivitamin, or scarfed down a yogurt before heading out the door this morning, you likely ingested non-nutritive sweeteners in the process. Non-nutritive sweeteners are substances that provide sweet taste but contribute few or no calories. While non-nutritive sweeteners were, until recently, found primarily in reduced-calorie “diet” foods and beverages, they are now widely present in foods, medications, and personal care products as well as in a variety of foods and beverages not marketed for weight management. Several non-nutritive sweeteners (e.g. acesulfame-potassium, aspartame, saccharin, stevia, sucralose, etc.) are approved by the U.S. Food & Drug Administration [Figure 1]. Whether they are helpful or harmful in the prevention and management of obesity and cardiometabolic diseases is controversial.
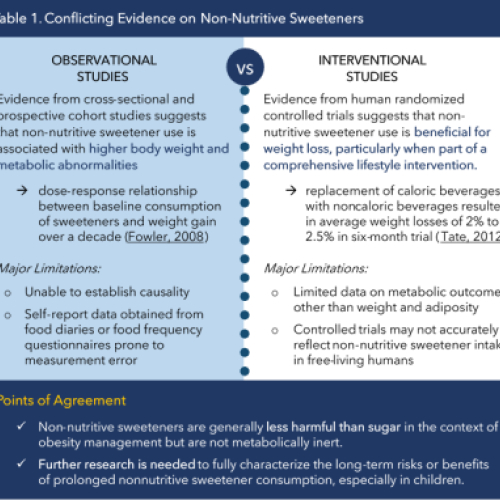
The prevalence of non-nutritive sweetener consumption is higher among persons with obesity relative to the general population. Although replacement of added sugars with non-nutritive sweeteners reduces the calorie content of foods and beverages, consumption of non-nutritive sweeteners may not lower total daily calorie and sugar intakes [Table 1]. Findings of observational studies demonstrate that consumption of non-nutritive sweeteners is consistently associated with higher energy intake, weight gain, and increased risk of cardiometabolic disease, and the observational studies are supported by mechanistic studies in animal models. However, the majority of randomized controlled trials (RCTs) in humans demonstrate neutral or beneficial effects of non-nutritive sweetener consumption on body weight.
The discordant findings between RCTs and observational studies may be explained by a number of factors, including limitations in study design and challenges in interpretation of study findings. For example, the association between sweetener consumption and weight gain may be because individuals already predisposed to obesity consume more sweeteners in attempts to prevent weight gain (reverse causality). There may also be unmeasured, unexplained factors that mediate or moderate the relationship between sweetener consumption and weight-related metabolic outcomes (residual confounding), such as whether non-nutritive sweeteners are consumed at the same time as sugary foods. Data from mouse and human models suggest that sweeteners could plausibly influence human metabolic processes by changing the gut microbiome, stimulating insulin secretion, increasing fat cell production, and/or changing taste preferences.
Global efforts to reduce sugar intake and prevent obesity have fueled marked increases in non-nutritive sweetener consumption in recent decades, based largely on the premise that replacing sugar with non-nutritive sweeteners will benefit energy balance. The upward trend in non-nutritive sweetener consumption is likely to continue as new policies inspire companies to reformulate popular, high-sugar items in their food and beverage portfolios. For example, last year Coca-Cola rapidly replaced half the sugar in its Sprite and Fanta with non-nutritive sweeteners to shield these products from the 18% tax and foreboding warning label required on high-sugar beverages under a new Chilean law.
Additional well-controlled, long-term intervention studies are needed to determine the effects of non-nutritive sweeteners on weight, adiposity and chronic disease in humans under free-living conditions and to inform policy and reformulation efforts. Neutral forums that allow diverse stakeholders to engage in cross-disciplinary discussions and critically evaluate approaches to address added sugar intake – like the seminar series hosted at GW in 2018 – may expedite progress in this important area of research.