Despite the high prevalence of obesity among Americans, few health professionals receive adequate training in how to deliver effective care for people with obesity. Core concepts related to obesity care are underrepresented on licensing exams. While most educational institutions recognize the importance of improved provider training and education around chronic disease, fewer have integrated obesity-specific knowledge and skills into their curricula.
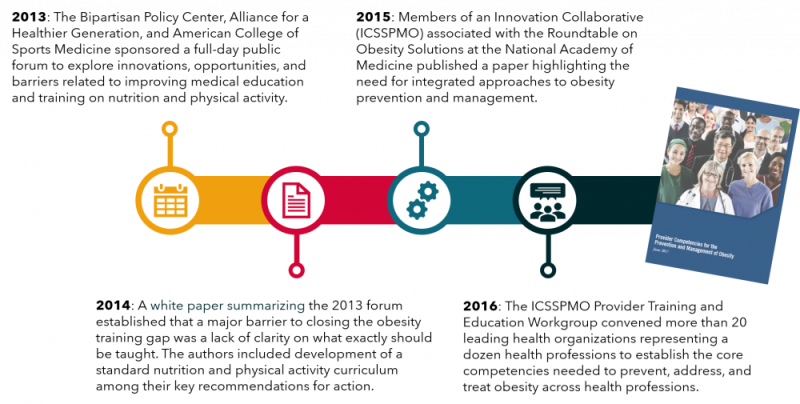
In recent years, STOP has intensified efforts to close the obesity training gap. In 2017, we helped to develop and disseminate the Provider Competencies for the Prevention and Management of Obesity (“the Competencies”), the first-ever interprofessional obesity care competencies designed to equip frontline providers with a common set of knowledge, skills, and attitudes essential for optimal care of clients with obesity (Figure 1). In 2018, we interviewed and convened key stakeholders to identify how training and education on obesity can be integrated into the curricula and care delivery practices of various health professions.
FIGURE 1. History of the Obesity Care Competencies
In 2019, we continued to address known resource gaps by curating a collection of Competency-aligned curricular materials and tools that can support organizational efforts to bolster provider training and education on obesity. Activities from the past year are briefly summarized below.
Survey of Health Professional Training Programs: Prior studies have identified gaps in the curricula of medical schools and residency programs, but less is known about how obesity is addressed in the formative training of non-physician providers. We conducted a nationwide curricular survey to assess how obesity is currently addressed in the pre-licensure training of various health professions that care for people with obesity. Programs that responded to the survey were most likely to address competencies related to core obesity knowledge (e.g. epidemiology of obesity) and least likely to address skills for interprofessional collaboration in obesity care.
Curricular Case Studies: Workgroup members indicated that training programs may benefit from examples of how provider training and education on obesity can be integrated in prelicensure curricula. We developed an interprofessional curricular case series that showcases real-world obesity competency integration strategies. Each case study highlights a program or institution that has incorporated one or more of the Competencies in its efforts to equip students, trainees, and/or practicing health professionals with the skills and knowledge needed to care competently and compassionately for persons with obesity.
Catalog of Curricular Resources: During our formative research, key stakeholders identified implementation toolkits with curricular frameworks and materials as resources that would most improve their profession’s ability to adopt the Competencies. To address this need, we created a database of Competency-aligned curricular materials, studies, and other resources that can be used to improve health professionals’ competence in caring for persons with obesity.
Perpetuation of a health workforce unprepared to care competently and compassionately for people with obesity is detrimental to population health outcomes and costly to health systems. Patients with obesity are shortchanged at nearly every turn in our current health system, from being denied for joint replacements to suboptimal dosing for essential drugs (e.g. anesthetics, emergency contraception). Simply educating providers on the genetic, physiological, psychological, environmental and social contributors to obesity may reduce the impact of weight stigma on quality of care.
Integration of competency-based training and education on obesity into existing curricula, continuing education, and possibly licensing exams is a foundational step toward a more effective, efficient 21st-century health system. Our hope is that these resources might inspire leaders in each profession to prioritize obesity education across their continuum of training. We encourage you to explore the Obesity Care Competencies website and to reach out to the STOP Team (obesity![]() gwu [dot] edu (obesity[at]gwu[dot]edu)) with questions, concerns, or comments.
gwu [dot] edu (obesity[at]gwu[dot]edu)) with questions, concerns, or comments.