Download: Fast Facts - Obesity and AI/AN Populations (PDF)
OBESITY is a complex chronic disease in which abnormal or excessive accumulation of body fat impairs health. Adult obesity rates have more than doubled since the 1980s — in the U.S. today, obesity affects over 42% of adults and 18% of youth.1,2 Obesity and its related complications are major drivers of rising healthcare costs, diminished health-related quality of life, and the recent decline in U.S. life expectancy. This fact sheet is part of a series designed to provide basic information about the science of obesity and current strategies to address it.
Key Takeaways
- American Indian/Alaska Natives face one of the highest rates of obesity and increased obesity-related mortality compared to other races.
- Colonialism and the displacement of AI/AN tribes led to the disruption of food systems, but there are current efforts to embrace indigenous foods.
- Efforts to diminish obesity rates should prioritize systemic, community-led, culturally relevant change for the most effective and lasting results.
Obesity Prevalence Among AI/AN Populations
American Indian/Alaska Natives (AI/ANs) experience one of the highest rates of obesity across all racial and ethnic groups in the U.S.3 Disparities in obesity prevalence also coincide with disparities in life expectancies and mortality for AI/AN populations.
- AI/ANs make up 1.7% of the total U.S. population. As of 2019, an estimated 5.7 million people identified as AI/AN alone or in combination with one or more other races. 4
- In 2018, 48.1% of AI/AN adults aged 18 and over had obesity. 5
- AI/AN adults are approximately 60% more likely to have obesity than non-Hispanic White adults.6
- The prevalence of obesity among AI/AN children is consistently higher than the prevalence for U.S. children overall.7
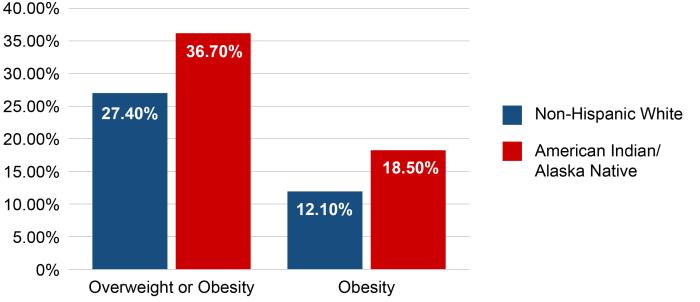
- In 2015, the prevalence of obesity in AI/AN children aged 2-19 was 29.7%.8 Among children ages 2 through 4 enrolled in the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) in 2016, AI/AN children experienced much higher prevalence of overweight and obesity compared to NonHispanic White children.9
- AI/AN individuals born in 2019 have a life expectancy that is 5.5 years less than the U.S. average for all races (73.0 years versus 78.5 years).10
- AI/AN populations experience higher mortality rates due to obesity-related conditions such as heart disease, diabetes, stroke, and chronic liver disease and cirrhosis compared to all U.S. races.10
Prevalence of Overweight and Obesity Among Children Ages 2-4 Enrolled in WIC, 2016
Risk Factors for Obesity in AI/AN Communities
Various upstream factors have contributed to the disproportionately high rates of obesity in AI/AN communities. Many of these are historically rooted, systemic inequities that continue to perpetuate adverse health effects on these communities today. These factors include:
- Food insecurity – historically, the forced relocation of AI/AN peoples away from their ancestral lands and onto reservations severely restricted their access to traditional, regionally-specific food systems such as hunting, gathering, fishing, and farming.11
- Many tribes were agriculturalists, and they originated the concept of regenerative agriculture. One example is seen in the Iroquois’ cultivation of the “Three Sisters” (corn, beans, and squash).12
- This disruption of indigenous food systems has resulted in dependence on federal government programs which include unhealthy foods.11 While AI/AN communities have adapted to these systemic changes – inventing new traditional foods such as fry bread13 – inconsistent funding for these food assistance programs and other social services continue to contribute to food insecurity.14
- AI/AN tribal area populations are mostly rural and experience high rates of poverty, resulting in restricted geographic and economic access to food.15
- Barriers in accessing and navigating health care services, including:
- Geographical isolation of rural areas, the costs of travel, and/or lack of access to transportation.16
- Unemployment, poverty, and lower rates of insurance coverage among AI/AN populations.16
- The underfunding of the Indian Health Service (IHS), which contributes to staff shortages and prolonged wait times in IHS clinics.16
Recommendations to Reduce Obesity and Comorbidities for AI/AN Communities
There exist many proposed solutions to the inequities that AI/AN communities experience. Recommendations include:
- Recognize and address the historical trauma that AI/AN tribes have faced. It is critical that we recognize the lasting impact of systemic racism while honoring the strength and resiliency of AI/AN communities.17-18
- Restore the cultural tradition of physical activity. Historically, tribes such as several Pueblo and Navajo chapters ran long distances on a regular basis. Restoring this cultural tradition via investment in community-led strategies can improve physical activity rates and help control obesity.19
- Improve research efforts to gather more comprehensive, accurate data on AI/AN population health, including further research on food insecurity in rural AI/AN communities. Research can then inform policy decisions to improve the health of AI/AN communities.11,14
- Engage with communities to conduct community-based participatory research and implement culturally relevant programs to promote local food production and increase food security.11,14, 20
- Promote food sovereignty, embrace indigenous diets, and improve access to traditional foods.11,21-22
- Promote early childhood nutrition through culturally tailored programs.11
- Tax unhealthy foods and subsidize healthier options.11
- Increase funding for the IHS and enable greater tribal control of health programs and services.16
- References
-
- Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity and severe obesity among adults: United States, 2017–2018. NCHS Data Brief, no 360. Hyattsville, MD: National Center for Health Statistics. 2020
- Hales CM, Carroll MD, Fryar CD, Ogden CL. Prevalence of obesity among adults and youth: United States, 2015–2016. 2017.
- KFF. Adults Who Are Obese by Race/Ethnicity. KFF. https://www.kff.org. Published November 2, 2021. Accessed November 15, 2021.
- Office of Minority Health. Profile: American Indian/Alaska Native. American Indian/Alaska Native - The Office of Minority Health. https://minorityhealth.hhs.gov/. Published 2021. Accessed November 15, 2021.
- NCHS. Summary Health Statistics: CDC National Health Interview Survey, 2018. 2018.
- OMH. Obesity and American Indians/Alaska Natives. The Office of Minority Health. https://minorityhealth.hhs.gov/. Published 2020. Accessed November 15, 2021.
- Hearst MO, Biskeborn K, Christensen M, Cushing C. Trends of overweight and obesity among white and American Indian School Children in South Dakota, 1998-2010. Obesity. 2013;21(1):E26-E32. doi:10.1002/oby.20022
- Bullock A, Sheff K, Moore K, Manson S. Obesity and overweight in American Indian and Alaska native children, 2006–2015. American Journal of Public Health. 2017;107(9):1502-1507. doi:10.2105/ajph.2017.303904
- Pan L, Freedman DS, Park S, et al. Changes in obesity among US children aged 2 through 4 years enrolled in WIC during 2010-2016. JAMA. 2019;321(23):2364-2366. doi:10.1001/jama.2019.5051
- IHS. Disparities: Fact sheets. Indian Health Service. https://www.ihs.gov/newsroom/factsheets/disparities/. Published October 2019. Accessed November 15, 2021.
- Warne D, Wescott S. Social Determinants of American Indian Nutritional Health. Curr Dev Nutr. May 2019:12-18. doi:10.1093/cdn/nzz054
- Heim T. The Indigenous Origins of Regenerative Agriculture. National Farmers Union. https://nfu.org/2020/10/12/the-indigenous-origins-of-regenerative-agriculture/. Published October 12, 2020. Accessed November 15, 2021.
- Maillard KN. Fry bread is beloved, but also divisive. The New York Times. https://www.nytimes.com/2021/11/01/dining/indigenous-people-fry-bread.html. Published November 1, 2021. Accessed November 15, 2021.
- Blue Bird Jernigan V, Salvatore AL, Styne DM, Winkleby M. Addressing food insecurity in a Native American reservation using community-based participatory research. Health Education Research. 2011;27(4):645-655. doi:10.1093/her/cyr089
- Kaufman P., Dicken C., Williams R. Measuring Access to Healthful, Affordable Food in American Indian and Alaska Native Tribal Areas. USDA: Economic Research Service. 2014;131.
- Cromer KJ, Wofford L, Wyant DK. Barriers to healthcare access facing American Indian and Alaska Natives in rural America. Journal of Community Health Nursing. 2019;36(4):165-187. doi:10.1080/07370016.2019.1665320
- Natividad I. In the fight for racial justice, Native stories should not be ignored. Berkeley News. https://news.berkeley.edu/2020/09/25/in-the-fight-for-racial-justice-native-stories-should-not-be-ignored/. Published September 25, 2020. Accessed November 15, 2021.
- Seaman C. We Are Still Here. Medium. https://fellowsblog.ted.com/we-are-still-here-9a595523db33. Published August 31, 2016. Accessed November 15, 2021.
- Warne D, Roanhorse O. Investing in Native Community-Led Strategies to Improve Physical Activity. NAM Perspectives. 2015;5(4). doi:10.31478/201504b
- Graham M. Will a native-led initiative spur an agricultural revolution in rural Alaska? High Country News. https://www.hcn.org/issues/53.6/indigenous-affairs-agriculture-will-a-native-led-initiative-spur-an-agricultural-revolution-in-rural-alaska. Published May 28, 2021. Accessed November 15, 2021.
- Minassian L. Indigenous Foods: How Colonized Diets Have Made Native Nations Sick - and What's Being Done About It Today. Food Revolution Network. https://foodrevolution.org/blog/indigenous-foods-systems-food-sovereignty/. Published February 8, 2021. Accessed November 15, 2021.
- North American traditional Indigenous Food Systems. NATIFS. https://www.natifs.org/. Published June 24, 2021. Accessed November 15, 2021.
A product of the Strategies to Overcome & Prevent (STOP) Obesity Alliance at the Sumner M. Redstone Global Center for Prevention & Wellness.