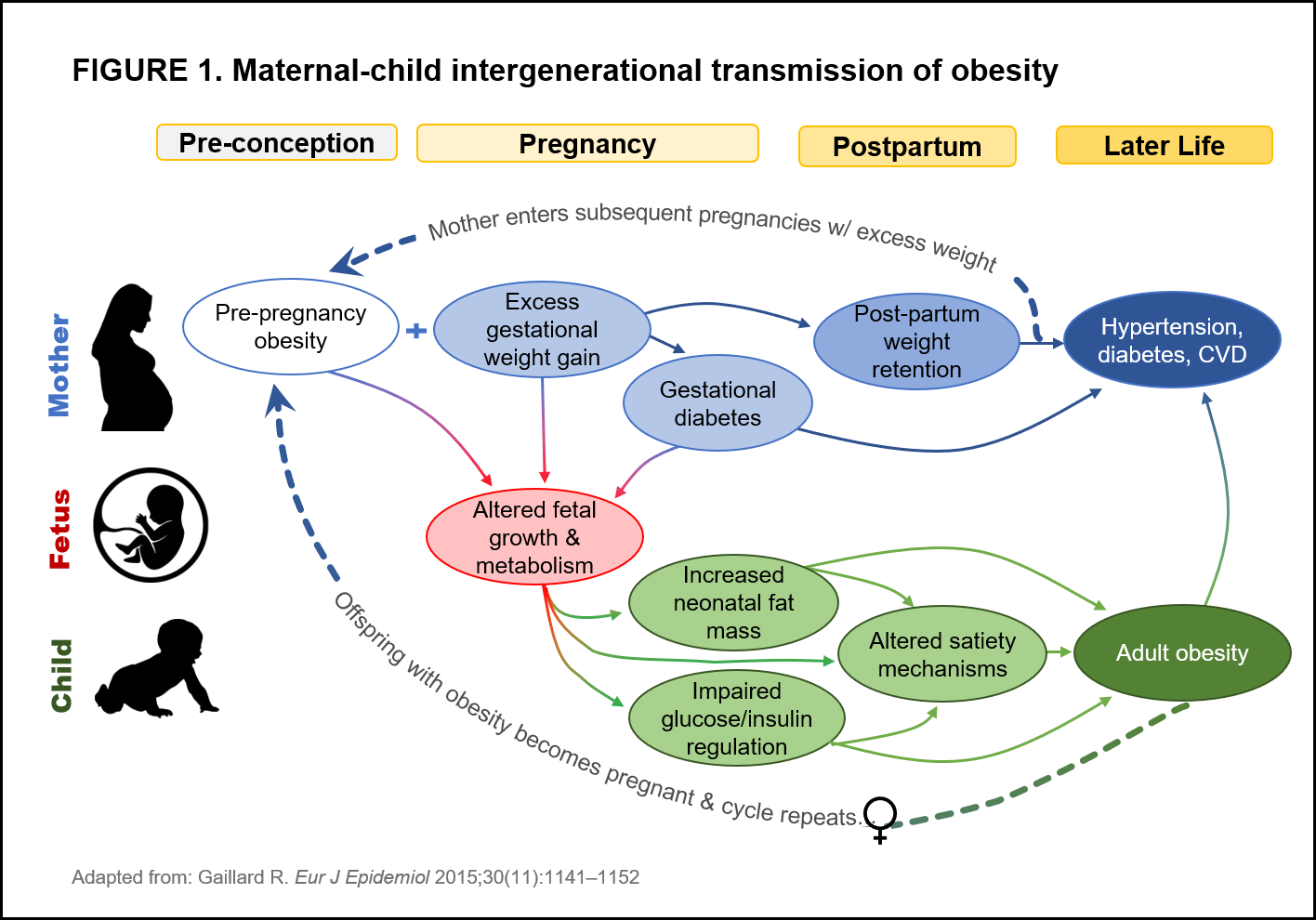
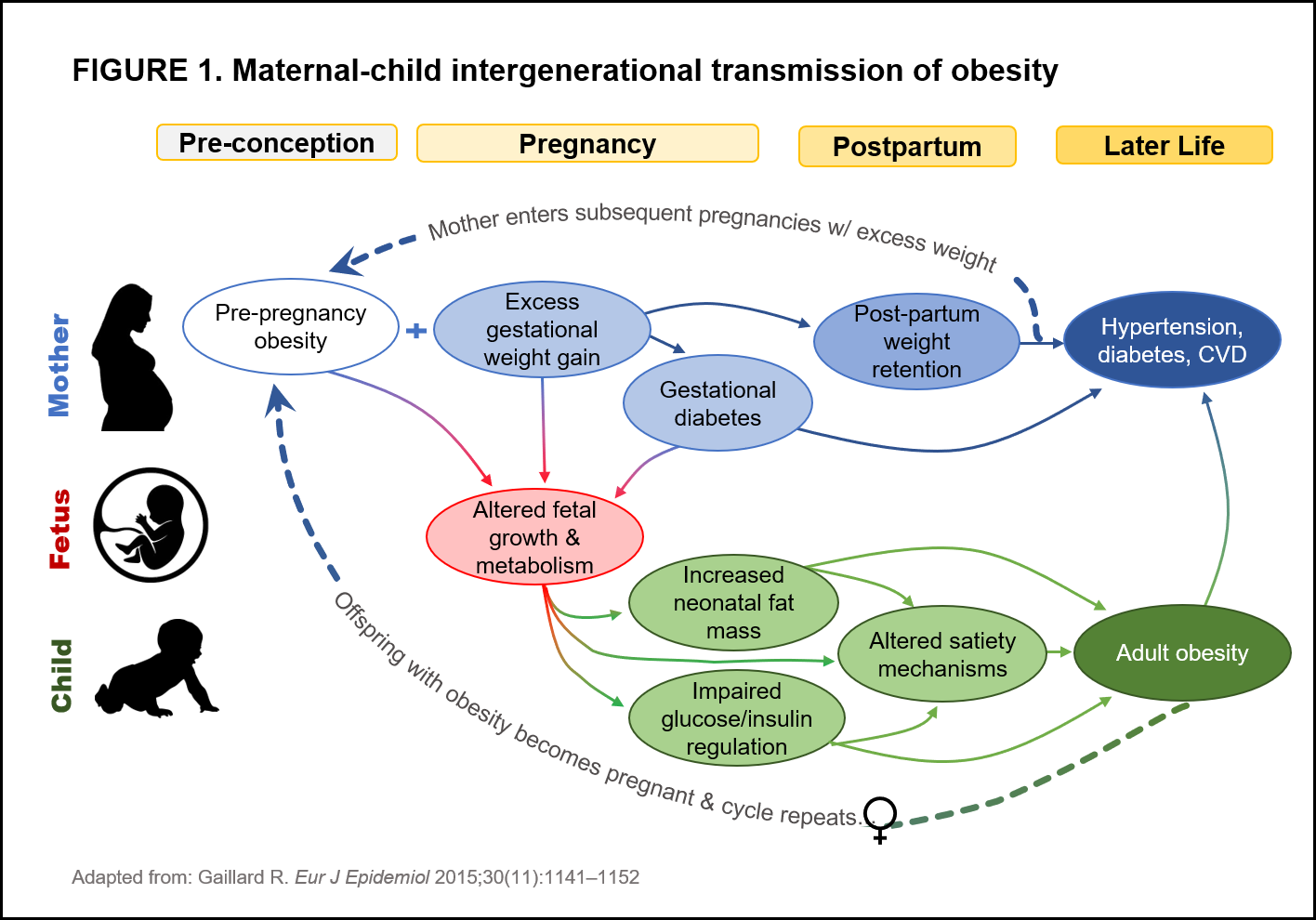
A growing body of evidence indicates that obesity has a detrimental impact on reproductive potential in women. In addition to reduced fertility, maternal pre-pregnancy body mass index (BMI), excessive gestational weight gain, and postpartum weight retention are collectively associated with adverse fetal development, obstetric complications, and long-term health outcomes for mothers and their offspring.