Obesity is driven by a wide range of interconnected causes, ranging from systems-level good food access to individual genetic predispositions. As researchers continue to understand how these contributors interact, there has been little emphasis on food noise, or constant intrusive thoughts about food that impact daily life. Weight Watchers and the STOP Obesity Alliance collaborated on a study to better understand food noise and how it impacts people with overweight and obesity.
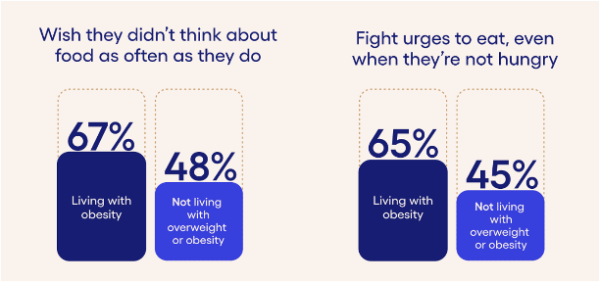
“Beyond Hunger: Understanding Food Noise” explores how 57% of individuals living with overweight or obesity experience continuous and disruptive thoughts about food. Only 12% of this group were familiar with the term food noise. Food noise limits a person’s ability to stick with a nutrition or exercise program for weight loss and to make healthy choices because of the intensity and persistence of food noise. Intensity can vary due to an individual’s environment and learned behaviors in addition to their biology. Overcoming the roadblock of food noise is an important aspect of comprehensive obesity care and the mental health needs of patients should not be brushed over.
Source: Beyond Hunger: Understanding Food Noise
Internal mental health factors like food noise and self-judgment are only half of the battle that people with overweight and obesity face when it comes to stigma. The food noise report investigated perceptions of obesity from those who do not live with overweight or obesity. The majority of people without obesity agree that those living with obesity are not taking care of themselves and might need a “tough love” approach to motivate them to lose weight. People living with overweight or obesity are aware that people around them may be thinking these thoughts which can limit their desire to seek treatment through anti-obesity medications (AOMs). The report found that 59% of people without overweight or obesity have more respect for people who lose weight without medication than those who use medication. One in four people living with obesity avoid talking to their friends and family about AOMs and avoid asking their doctors about weight loss medications. Stigma from all corners of society leads to extra roadblocks for those seeking care to improve their health.
Anti-obesity medications, also known as GLP-1s (glucagon-like peptide 1 agonists), that act on satiety and reward pathways, can help to dramatically quiet food noise. As patients find themselves released from intrusive thoughts about food, many find it easier to focus on other priorities in their lives.
Source: Beyond Hunger: Understanding Food Noise
Anecdotal reports from patients using GLP-1s for weight loss point to even more interesting effects, like reduced cravings for alcohol and nicotine and reduced compulsive behaviors like excessive shopping and gambling. Further research is needed to understand the varying impacts of GLP-1s and their ability to treat other conditions linked to brain reward pathways, such as addiction.